Intracoronary Imaging
The Cardialysis Intracoronary Imaging Core Lab has extensive experience in analyzing stent trials as well as plaque progression/regression trials using classical imaging modalities such intravascular ultrasound (IVUS). There have been numerous landmark trials in this field such as the MUSIC, PERSPECTIVE, IBIS 2, APPROACH, ABSORB studies and RESOLUTE and LEADERS OCT substudies. To accomplish such endeavors, we have a network of more than 100 clinical sites that have been selected as our preferred choice based on their high-quality performance.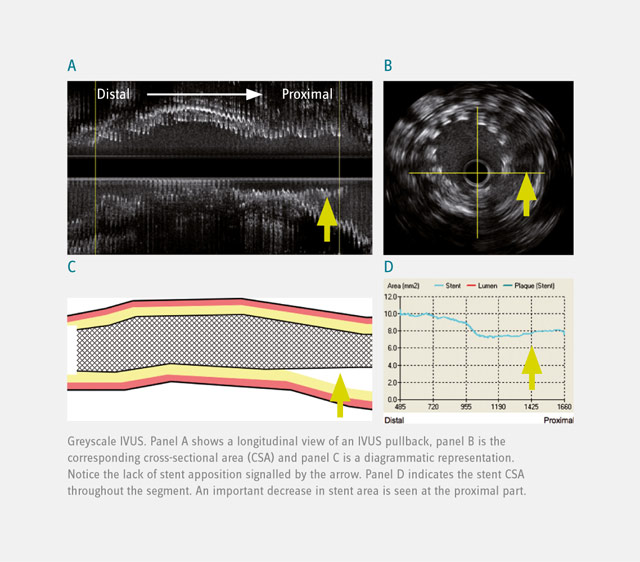
IVUS
Intravascular Ultrasound (IVUS) is a technique providing cross-sectional, high-resolution tomographic images of the arterial wall. This technique yields qualitative and quantitative assessment of the extent and severity of arterial atherosclerotic disease. By detecting luminal, external elastic membrane and stent boundaries, IVUS is able to quantify luminal area, vessel area, scaffold/stent area, plaque thickness, and area obstruction. In addition, quantitative and qualitative assessment of incomplete stent apposition enables evaluation of the efficacy of devices and pharmacotherapy.
Virtual Histology
IVUS Virtual Histology is an intravascular ultrasound derived color-coded plaque characterization technique. Compared to standard IVUS, this imaging modality allows a more detailed assessment of different plaque components. In preliminary in vitro studies, four plaque types (fibrous tissue, fibro-fatty tissue, necrotic core and dense calcium) as determined by histology could be correlated with a specific spectrum of the radiofrequency signal. This technique, given its ability to identify necrosis-rich plaques, is of great value in identifying potentially vulnerable plaque.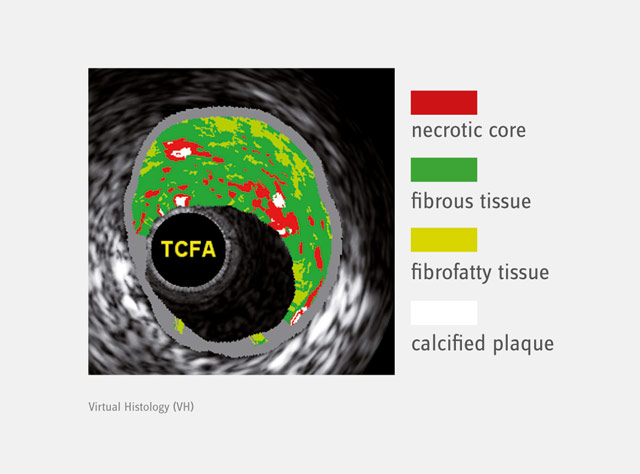
TVC Imaging System
Another imaging modality able to characterize coronary atherosclerosis (i.e. lipid core) invasively is the TVC (true vessel characterization) imaging system or NIR (near-infrared) spectroscopy. This imaging modality was used in the IBIS 3 trial; a study that was able to assess the effects of rosuvastatin on the content of necrotic core (IVUS-VH) and lipid-containing regions (NIRS) at 52 weeks.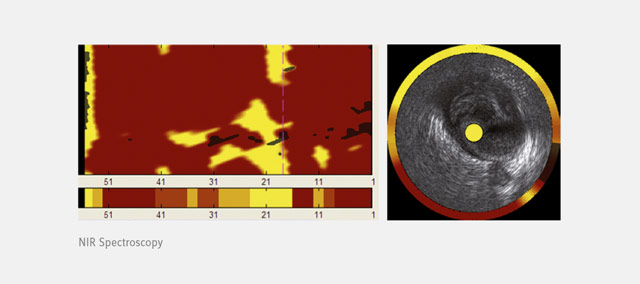
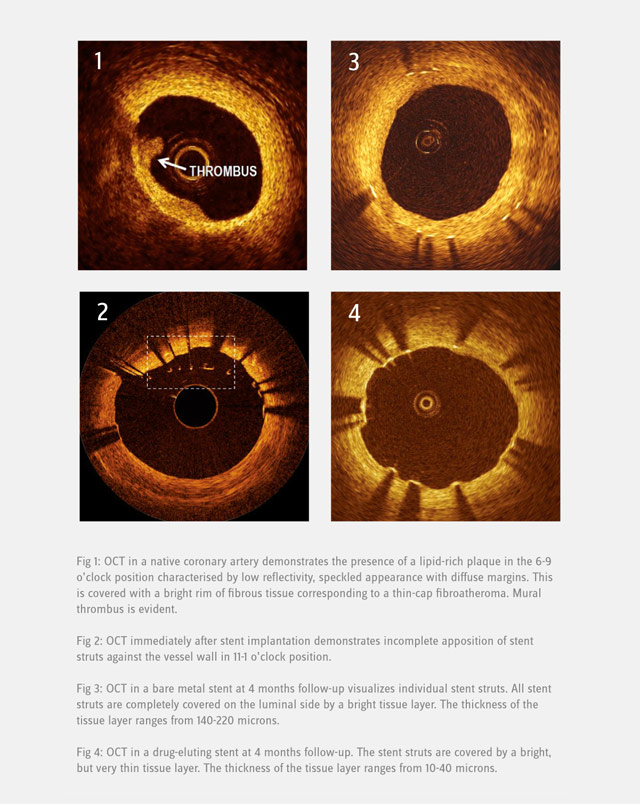
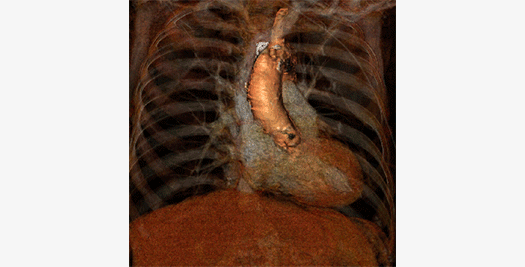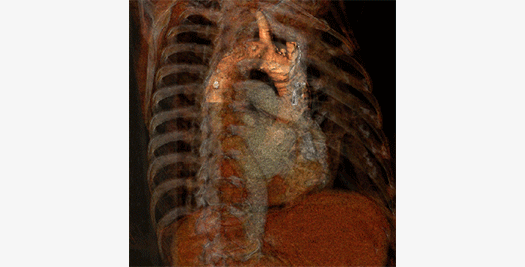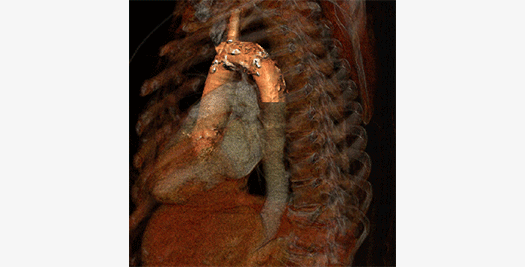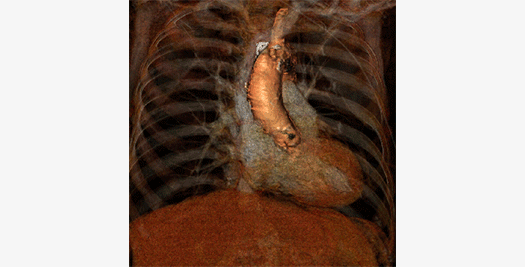
Optical Coherence Tomography
Optical Coherence Tomography (OCT) is a light-based imaging modality permitting the in-vivo visualization of biological tissues with an unmatched resolution of 15 microns. This unique capability has resulted in OCT being rapidly adopted and accepted in stent/scaffold studies with the ability to provide accurate assessment of their apposition and tissue coverage over individual stent/scaffold struts. Other exciting applications include the detailed assessment of the vessel wall and its structural changes over time together with the characterization of atherosclerotic plaque components. More recently, the introduction of three dimensional reconstructions has pushed this field forward. It helps us understand the interaction between vessel wall and coronary devices and offers the opportunity to serially assess the changes in a more comprehensive manner.
Such an approach ensures that maximum information is obtained from the clinical study evaluating a particular device and/or drug. Closely guided by clinical experts in the specific field, Cardialysis serves as a Core Lab for a variety of these imaging techniques.